MSA research at UNSW: Unravelling a genetic mystery
Supported by a community of MSA patients and their families, Dr Michael Janitz and his research team are pioneering solutions for early detection and treatment of this rare and misunderstood neurodegenerative disease.
The brain is our most complex organ, and arguably our most important. So how can we keep it healthy and running smoothly into old age? This is a fundamental question driving the research of Dr Michael Janitz, a geneticist at the UNSW School of Biotechnology and Biomolecular Sciences.
In Australia’s ageing society, Dr Janitz believes the focus on preventing neurodegenerative diseases is beginning to rival that of curing cancer, from a public health perspective. With help from many generous donors, the founder and Director of the UNSW Laboratory for Brain Transcriptomics wants to better understand the genetic factors that cause age-related brain diseases and cognitive decline.
To do so, he and his team of six researchers are peering inside brain cells to get a molecular-level understanding of gene expression, using tissue from healthy donors and comparing them to people with neurodegenerative diseases. Using sophisticated genetic sequencing techniques, Dr Janitz and his team are creating a reference for what constitutes ‘normal’ gene expression in healthy brains, and thus begin to search for deviations that might be symptomatic of diseases.
Dr Janitz is particularly interested in trying to untangle the genetic cause of a condition called multiple systems atrophy, or MSA. People often develop MSA in their 50s or 60s, and it can lead to progressive immobility as well as trouble breathing, talking, seeing and swallowing. There is currently no treatment for the debilitating disease.
“MSA is a rare neurodegenerative disease, affecting around 2,500 people in Australia, with a lack of early biomarkers to indicate its onset,” says Dr Janitz. Although it doesn’t have the same profile as Alzheimer’s or other dementias, it can be devastating for patients and families affected. Further, MSA is often mistaken for Parkinson’s disease, which can result in patients starting ineffective treatment programs, living with the worsening disease for years before getting a proper diagnosis.
The science behind success
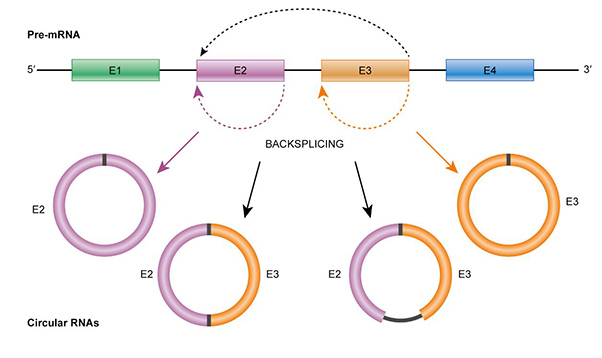
Dr Janitz believes circular RNAs hold the key for diagnosing MSA. When DNA instructions are copied into the gene expression process, an RNA molecule is produced. These act like messengers, transporting the instructions from the cell’s nucleus to one of the cell’s many protein-making factories, called ribosomes. Here, the RNA translates the instructions, and proteins are generated.
RNA molecules are typically shaped like straight lines, but sometimes they are converted to circular structures. In this form, they become non-coding RNAs, meaning they carry genetic instructions, but never translate them into proteins. Because they are more stable than their linear counterparts, however, they show up in the bloodstream.
“If we know which circular RNAs or circular lines we are looking for… we could actually just take a simple blood test to diagnose MSA,” says Dr Janitz. In a significant breakthrough, his team recently identified a potential circular RNA biomarker for MSA, enabling its early detection. The next step is getting statistical confirmation that it’s the right needle in the haystack.
A community of support
After being contacted by the family of an MSA patient three years ago, Dr Janitz was inspired to set up the MSA Research Fund at UNSW, which is crucial to support ongoing breakthroughs in this area. He has since also begun a dialogue with many members of the MSA community, offering support and information about research findings.
In response, the community have rallied to generously support his cutting-edge brain science. At this early stage, the goal isn’t to provide a cure or drug for the disease, cautions Dr Janitz. “What we are delivering is a long-term perspective that [the disease’s untreatable status] can change.”
As one of the very few Australian research laboratories studying MSA, Dr Janitz says his group is well-positioned to improve understanding about the disease and develop applied solutions. His goal is to develop a blood test for quick and early diagnosis, which he says would enable better management of the disease, and could one day lead to more effective treatments.
More immediately, he is motivated by providing hope to the people impacted by the disease: “My impression is that many MSA patients and their families feel a little bit abandoned in terms of the awareness and information available,” he says. “So my message to them is that we are here to specifically focus on this disease and to progress understanding.
“We are researchers,” he adds, “but we are always open to talking to people and trying to explain the problems and challenges. This is what we have been doing with MSA patients and families, and this is extremely important.”
For a full copy of the 2017 Donor Impact Report, click here.








